- Radiation Therapy After Lumpectomy
- Lumpectomy and Lymph Node Removal
- Additional Resources and References
Lumpectomy, also known as breast-conserving surgery, is the surgical removal of a cancerous lump (or tumor) in the breast, along with a small margin of the surrounding normal breast tissue. Lumpectomy may also be called wide excision biopsy, breast conserving therapy or quadrantectomy (this latter term is used when up to one fourth of the breast is removed). The procedure is often performed on women with small or localized breast cancers and can be an attractive surgical treatment option for breast cancer because it allows women to maintain most of their breast after surgery. Several studies have shown that women with small breast tumors have an equal chance of surviving breast cancer regardless of whether they have a lumpectomy, followed by a full course of radiation therapy, or mastectomy (complete breast removal, which generally does not require post-operative radiation treatment).
- Who is/is not a Candidate For Lumpectomy?
- How is Lumpectomy performed?
- Radiation Therapy After Lumpectomy
- Lumpectomy and Lymph Node Removal
- Additional Resources and References
After a patient has been diagnosed with breast cancer, physicians will stage the cancer to determine the extent of the disease and help decide the most appropriate course of treatment. Lumpectomy is often a suitable treatment option for patients with the following breast cancers:
- Ductal carcinoma in situ (DCIS)
- Stage I
- Stage II
- Stage III
![]() Click here to learn more about these types of breast cancers.
Click here to learn more about these types of breast cancers.
Lumpectomy involves removing the cancerous breast lump and a surrounding margin of normal breast tissue. In addition to the lumpectomy, a separate incision may be required to include a sampling or removal of the axillary (underarm) lymph nodes. This part of the surgery, which may be a sentinel node biopsy, an axillary lymph node sampling, or an axillary lymph node dissection, is performed to determine whether the cancer has begun to spread out of the breast itself (see the section below on lymph node removal for more information).
After the lumpectomy is performed, the pathologist will check to make sure the surgeon removed the entire cancerous tumor by seeing if the tissue margins are "clear" (in other words, if there is no cancer present in the outermost edges of the breast tissue sample). A preliminary check of the tissue margins may be performed while the patient is still in the operating room and may allow the surgeon to obtain "clear margins" during the same operation. However, this is only a preliminary reading, and the final results, available over the course of a few days, may reveal residual cancer cells (known as a "positive" margin). If the margins of the removed breast tissue do contain cancer cells, then additional surgery (re-excision) is usually necessary to attempt to remove the remaining cancer. If it is not possible to clear the margins on re-excision, then a mastectomy is usually offered as an alternative.
Lumpectomy is often combined with adjuvant (additional) therapy, either local or systemic. Most commonly, lumpectomy is followed by at least six weeks of radiation therapy to ensure that all cancer cells in the remaining breast have been destroyed. Newer studies are beginning to show that shorter radiation times may be equally effective in preventing local tumor recurrence for many patients after lumpectomy; however, this is still under investigation. Other types of adjuvant therapy that may be given in addition to lumpectomy include agents designed to help control the systemic spread of breast cancer. These agents include chemotherapy, the drug tamoxifen (brand name, Nolvadex), or a combination of hormonal or drug therapies.
Several studies have shown that lumpectomy is a viable treatment option for most women with small, localized breast cancers. In fact, there is no statistically significant difference in overall survival rates between women who undergo lumpectomy (and radiation) and those who undergo mastectomy, although a slightly higher local recurrence rate was reported in some larger studies in women who undergo lumpectomy instead of mastectomy. More recently, a large study conducted by Yale researchers found that women with very early-stage breast cancers who undergo lumpectomy followed by radiation therapy are no more likely to develop a second cancer than women who undergo mastectomy, as long as candidates are selected appropriately and the edges of the surgical sample are free of cancer cells.
There are some women who are not good candidates for lumpectomy. The American Cancer Society suggests that women who have already undergone radiation in the breast/chest area, women with two or more areas of cancer in the same breast (known as multicentric disease), women whose previous lumpectomy did not completely remove the cancer, women with connective tissue diseases such as scleroderma (which make tissue sensitive to radiation), or women who would be pregnant at the time of radiation therapy (possibly harming the fetus) should not consider lumpectomy as advisable treatment. In addition, women with cancers more than five centimeters in diameters (two inches) or women with larger cancers within relatively small breasts may not be suitable candidates for lumpectomy. The following chart summarizes conditions for which lumpectomy may not be the most suitable choice:
| Poor Candidates for Lumpectomy |
|
Source: American Cancer Society
Women who have been diagnosed with breast cancer should carefully discuss their treatment options with their surgeon and other members of their cancer treatment team. Lumpectomy is becoming an increasingly suitable option for many women with early stage breast cancers. While some women are clearly not candidates for lumpectomy (and would benefit more from mastectomy), studies have shown that the type of breast cancer surgery a patient receives is sometimes influenced by her surgeon’s personal preference, geographical location, age, or insurance coverage. It is very common and usually recommended that patients seek a second opinion before undergoing any type of surgery.
|
Rates of Breast-Conserving Surgery by U.S. Region | |
| Northeast North Central West South |
60.5% 51.1% 50.2% 48.0% |
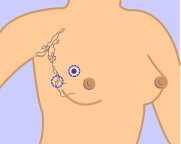 |
This illustration shows how lumpectomy is performed by removing the tumor and margin of surrounding normal breast tissue. Some of the axillary (underarm) lymph nodes may also be removed in patients who undergo lumpectomy. Illustration courtesy of theNCI/NIH. |
Lumpectomy may be performed using a local anesthetic, sedation, or general anesthesia, depending on the extent of the surgery needed. The surgeon makes a small incision over or near the breast tumor and excises (cuts free) the lump or abnormality along with a margin of at least one centimeter (approximately one half inch) of normal surrounding breast tissue (see the section above for information on margins). Unlike after mastectomy, a drainage tube is usually not necessary after lumpectomy.
A seroma (clear fluid trapped in the wound) usually fills the surgical cavity after the operation and helps to naturally remold the breast’s shape. Gradually, the seroma is absorbed and the body replaces it with scar tissue. This natural healing process and formation of scar tissue occurs over a period of months, so that the final results of the surgery may not be apparent for some time. Depending on such factors as the location of the mass, its initial size, the type of incision used, etc., the final result will be different for each person.
| Possible Side Effects of Lumpectomy Include: |
|
Patients are usually able to go home the same day or one to two days following lumpectomy. Most women are able to resume normal activities within two weeks. Wound infection or bleeding is not common with lumpectomy. The extent of breast soreness correlates with the amount and location of tissue removed during surgery, whether axillary (underarm) lymph node surgery was performed, and an individual’s tolerance to pain. Major soreness usually ceases after two to three days and should be checked by a physician if there is any increase in pain over time. Because lumpectomy is usually intended to preserve the cosmetic appearance of the breast, surgeons generally do not recommend lumpectomy when over one fourth of the breast must be removed. In these cases, mastectomy, along with the option of reconstruction, may be preferable.
In rare instances, women may experience recurring seromas after lumpectomy. Seromas are collections of fluid in the cavity (empty space) left behind by the surgery. These collections are easily drained (aspirated) in the surgeon’s office. If a seroma recurs, surgeons may use several methods including compression or sclerosis (the injection of ethanol, autologus fibrin clot, or fibrin sealant) to fill and harden the space in the breast. At times, these treatments can be uncomfortable, but they are rarely needed.
Lumpectomy (and sometimes mastectomy) is typically followed by six to seven weeks of radiation therapy immediately following surgery to help ensure that any remaining cancer cells are destroyed and to help prevent the chance of a cancer recurrence. Treatment with radiation usually begins one month after surgery, allowing the breast tissue adequate time to heal. Treatments are given daily and each treatment generally lasts a few minutes; the entire radiation session after machine set-up typically lasts 15 to 30 minutes. The procedure itself is pain-free. While the radiation is being administered, the technologist will leave the room to monitor the patient on a closed-circuit television. However, patients should be able to communicate with the technologist at any time over an intercom system.
| Common Side Effects of Radiation Therapy |
|
Most of the side effects associated with radiation therapy are temporary, and many patients do not experience significant discomfort after radiation sessions.
Researchers have been investigating whether a shorter duration, higher dose of radiation may be as effective as the conventional six to seven week regimen. Recent research suggests that limiting radiation therapy to four weeks at a higher dose may be as effective as the traditional regimen and could reduce side effects. IMRT (intensity-modulated radiation therapy) uses a highly sophisticated system of delivering external-beam radiation. According to recent research, this system uses advanced computer optimized planning and radiation delivery techniques that create more optimal dose distributions, greater sparing of the skin and lower doses to organs such as lung and heart--thus reducing potential side effects. However, there may be patients who are uncomfortable with the idea of an accelerated treatment and want to be treated with a more conventional six to seven week course of treatment. "In addition, we need more research to determine which women are ideal candidates for this treatment because of differences in anatomy or other treatments for their breast cancer." Women are encouraged to talk to their cancer treatment team about their radiation therapy options.
Click here for more information on radiation therapy.
 |
|
|
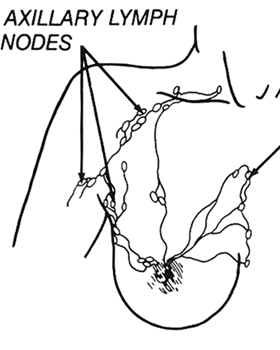
When breast cancer cells begin to escape from the primary tumor site in the breast, they first travel to the lymph nodes under the upper arm. Therefore, it is often necessary to remove some or all of the axillary (underarm) lymph nodes during lumpectomy or mastectomy to determine if or to what extent the cancer has spread.
Lymph node removal usually requires a separate incision when it is performed during the same procedure as lumpectomy. There are two procedures for removing lymph nodes in breast cancer patients: axillary node dissection and sentinel node biopsy.
- Axillary node dissection: This is the standard way to remove axillary lymph nodes. Typically, between 10 to 30 lymph nodes are removed and examined in a pathology laboratory to determine whether they contain cancer cells.
- Sentinel lymph node biopsy: This is a technique that involves the injection of a blue dye, radioactive tracer, or both, to identify the "sentinel" lymph nodes (first nodes) draining the breast. Using this method, only the first one to three lymph nodes in the lymphatic chain are removed. Research has shown that checking the sentinel lymph nodes allows physicians to accurately determine whether the axillary (armpit) lymph nodes contains cancer while causing fewer side effects such as lymphedema (chronic swelling) of the arm. If the sentinel nodes are positive (contain cancer cells), then additional surgery is performed to remove (dissect) the remaining axillary lymph nodes. If the removed axillary lymph nodes are negative (do not contain cancer cells), then no additional lymph nodes are removed, reducing the side effects of axillary dissection. Sentinel lymph node biopsy has become more common in recent years. However, it is not always appropriate. Click here for more information about this procedure.
The most common side effect of lymph node removal is lymphedema (chronic swelling) of the arm. Between 10% and 20% of patients who have lymph nodes remove develop lymphedema, including some patients who only have a sentinel lymph node biopsy. The risk of lymphedema is greater if the patient also undergoes radiation therapy and/or the lymph nodes contained cancer cells upon final examination. To help manage lymphedema and prevent long-term suffering, patients should report symptoms as soon as they occur. In addition, special exercises should be performed shortly after recovering from surgery to help encourage and maintain lymphatic flow of the affected side of surgery.
|
Early Signs of Lymphedema |
|
In addition to lymphedema, other common side effects of lymph node removal include limitations of arm/shoulder movement, and numbness of the upper arm skin. Click here to learn more about lymphedema.
- The American Cancer Society, http://www.cancer.org, provides detailed information on lumpectomy and other breast cancer treatment options.
- O’Grady, Lois et al, A Practical Approach to Breast Disease, Boston: Little Brown and Company, 1995.
- To learn more about radiation therapy, please visit http://www.imaginis.com/breasthealth/radio_bctreatment.asp
- To learn more about lymphedema, please visit http://www.imaginis.com/breasthealth/lymphedema.asp
Updated: December 29, 2009



