- How Breast MRI is Performed
- Benefits of an MRI Exam of the Breast
- Limitations to an MRI Exam of the Breast
MRI has several potential benefits in helping to investigate breast concerns. An MRI exam allows breast images to be taken in any plane and from any orientation. One particular advantage of MRI is that it is highly sensitive to small abnormalities that can sometimes be missed with other exams. For instance, a mammogram or ultrasound (sonogram) of the breast may reveal breast cancer in one area. However, an MRI of the breast may show that the cancer is in fact multi-focal; small tumors are present in several areas of the breast. Researchers are currently investigating whether MRI would be helpful to routinely use on breast cancer patients to screen for cancer in the opposite breast. Determining the extent of breast cancer with MRI can help indicate treatment: breast conserving surgery (lumpectomy) or breast removal (mastectomy). Mastectomy is indicated if there are multiple tumors.
MRI may also be useful in helping to determine whether breast cancer has spread into the chest wall. If there is evidence of breast cancer in the chest wall, a patient often needs to undergo chemotherapy before breast cancer surgery. Not knowing whether the chest wall is involved can delay chemotherapy and cause the patient to have both chemotherapy and radiation therapy after surgery. Physicians sometimes use MRI to detect cancer recurrences in women who have already been treated for breast cancer with lumpectomy.
In addition, MRI can assess whether a newly inverted nipple is evidence of a retroareolar cancer, a tumor under the areola (the pigmented region surrounding the nipple).
Another major benefit of MRI is that it plays a significant role in the visualization of breast implants. MRI can often show if an implant is leaking or ruptured. MRI can also image the breast tissue that is compressed by an implant. Implants can obscure some of the breast tissue on conventional mammogram images, making abnormalities or sings of cancer more difficult to see. This is because the x-rays used for mammography cannot penetrate silicone or saline implants well enough to image the overlying or underlying breast tissue. MRI imaging does not have this limitation. However, mammography is still the best tool for evaluating breast tissue and for screening for breast cancer. There is currently no routine recommendation for using MRI as a cancer screening tool in women with implants, although it can be helpful in selected cases.
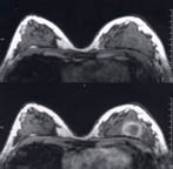
Transverse fast acquisition breast MRI images at same level without contrast (upper) and with contrast (lower). Note how the abnormality in the lower breast image on the right is "highlighted" by the contrast (Gadolinium DTPA).
Because MRI is very sensitive, the American Cancer Society recently recommended that women at very high risk of developing breast cancer have annual breast MRI exams in addition to annual mammograms to increase the likelihood that breast cancer will be detected early. While most women under 40 years of age do not require any breast imaging (i.e., mammography), some younger women are at high risk of breast cancer due to a strong family history or a mutated breast cancer gene (BRCA1 or BRCA2). However, young women tend to have dense breast tissue which can make screening mammography less effective. This is because breast tissue density shows up as a white region on a mammogram just as a cancer would. (As women age, their breasts become less dense, increasing the effectiveness of screening mammography). With MRI, physicians may be able to more easily distinguish between density and breast abnormalities.
The American Cancer Society recommends breast MRI exams for women with one of the following:
- a BRCA1 (breast cancer gene 1) or BRCA2 (breast cancer gene 2) mutation
- a first-degree relative (parent, sibling, child) with a BRCA1 or BRCA2 mutation, even if they have yet to be tested themselves --a lifetime risk of breast cancer oft 20%-25% or greater, based on one of several accepted risk assessment tools that consider family history and other factors -a history of radiation to the chest between the ages of 10 and 30
- Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or may have one of these syndromes based on a history in a first-degree relative
Women should consult their physicians to determine their lifetime breast cancer risk.
Benefits of Breast MRI
- Can image breast implants and ruptures
- Highly sensitive to small abnormalities
- Used effectively in dense breasts
- Can evaluate inverted nipples for evidence of cancer
- Can evaluate the extent of breast cancer
- Can help determine what type of surgery is indicated (lumpectomy or mastectomy)
- May detect breast cancer recurrences and residual tumors after lumpectomy
- Can locate primary tumor in women whose cancer has spread to axillary (armpit) lymph nodes
- Can spot or characterize small abnormalities missed by mammography
- May be useful in screening women at high risk for breast cancer, according to recent studies



