It is important for women to become familiar with the normal anatomy and physiology (function) of their breasts so that they can recognize early signs of possible abnormalities. This section outlines basic information on breast composition, development, and typical changes from puberty to pregnancy to menopause.
The breast is a mass of glandular, fatty, and fibrous tissues positioned over the pectoral muscles of the chest wall and attached to the chest wall by fibrous strands called Cooper’s ligaments. A layer of fatty tissue surrounds the breast glands and extends throughout the breast. The fatty tissue gives the breast a soft consistency.
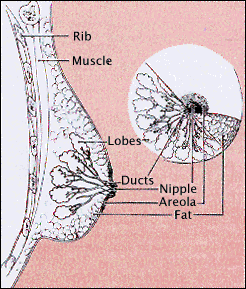
Image courtesy of NCI/NIH
The glandular tissues of the breast house the lobules (milk producing glands at the ends of the lobes) and the ducts (milk passages). Toward the nipple, each duct widens to form a sac (ampulla). During lactation, the bulbs on the ends of the lobules produce milk. Once milk is produced, it is transferred through the ducts to the nipple.
The breast is composed of:
- milk glands (lobules) that produce milk
- ducts that transport milk from the milk glands (lobules) to the nipple
- nipple
- areola (pink or brown pigmented region surrounding the nipple)
- connective (fibrous) tissue that surrounds the lobules and ducts
- fat
Arteries carry oxygen rich blood from the heart to the chest wall and the breasts and veins take de-oxygenated blood back to the heart. The axillary artery extends from the armpit and supplies the outer half of the breast with blood; the internal mammary artery extends down from neck and supplies the inner portion of the breast.
Human breast tissue begins to develop in the sixth week of fetal life. Breast tissue initially develops along the lines of the armpits and extends to the groin (this is called the milk ridge). By the ninth week of fetal life, it regresses (goes back) to the chest area, leaving two breast buds on the upper half of the chest. In females, columns of cells grow inward from each breast bud, becoming separate sweat glands with ducts leading to the nipple. Both male and female infants have very small breasts and actually experience some nipple discharge during the first few days after birth.
Female breasts do not begin growing until puberty—the period in life when the body undergoes a variety of changes to prepare for reproduction. Puberty usually begins for women around age 10 or 11. After pubic hair begins to grow, the breasts will begin responding to hormonal changes in the body. Specifically, the production of two hormones, estrogen and progesterone, signal the development of the glandular breast tissue. This initial growth of the breast may be somewhat painful for some girls. During this time, fat and fibrous breast tissue becomes more elastic. The breast ducts begin to grow and this growth continues until menstruation begins (typically one to two years after breast development has begun). Menstruation prepares the breasts and ovaries for potential pregnancy.
| Before puberty | Early puberty | Late puberty |
| the breast is flat except for the nipple that sticks out from the chest | the areola becomes a prominent bud; breasts begin to fill out | glandular tissue and fat increase in the breast, and areola becomes flat |
The size and shape of women’s breasts varies considerably. Some women have a large amount of breast tissue, and therefore, have large breasts. Other women have a smaller amount of tissue with little breast fat.
Factors that may influence a woman’s breast size include:
- Volume of breast tissue
- Family history
- Age
- Weight loss or gain
- History of pregnancies and lactation
- Thickness and elasticity of the breast skin
- Degree of hormonal influences on the breast (particularly estrogen and progesterone)
- Menopause
A woman’s breasts are rarely balanced (symmetrical). Usually, one breast is slightly larger or smaller, higher or lower, or shaped differently than the other. The size and characteristics of the nipple also vary greater from one woman to another. In some women, the nipples are constantly erect. In others, they will only become erect when stimulated by cold or touch. Some women also have inverted (turned in) nipples. Inverted nipples are not a cause for concern unless the condition is a new change. Since there are hair follicles around the nipple, hair on the breast is not uncommon.
The nipple can be flat, round, or cylindrical in shape. The color of the nipple is determined by the thinness and pigmentation of its skin. The nipple and areola (pigmented region surrounding the nipple) contain specialized muscle fibers that respond to stimulation to make the nipple erect. The areola also houses the Montgomery’s gland that may appear as tiny, raised bumps on the surface of the areola. The Montgomery’s gland helps lubricate the areola. When the nipple is stimulated, the muscle fibers will contract, the areola will pucker, and the nipples become hard.
Breast shape and appearance undergo a number of changes as a woman ages. In young women, the breast skin stretches and expands as the breasts grow, creating a rounded appearance. Young women tend to have denser breasts (more glandular tissue) than older women.
On mammogram films, breast masses, including both non-cancerous and cancerous lesions, appear as white regions. Fat appears as black regions on the films. All other components of the breast (glands, connective tissue, tumors, calcium deposits, etc.) appear as shades of white on a mammogram. In general, the younger the woman, the denser her breasts. As a woman ages, her breasts become less dense and the space is filled with fatty tissue shown as dark areas on mammography x-rays. It is usually easier for radiologists to detect breast cancer in older women because abnormal areas are easier to spot.
During each menstrual cycle, breast tissue tends to swell from changes in the body’s levels of estrogen and progesterone. The milk glands and ducts enlarge, and in turn, the breasts retain water. During menstruation, breasts may temporarily feel swollen, painful, tender, or lumpy. Physicians recommend that women practice monthly breast self-exams the week following menstruation when the breasts are least tender.
Fibrocystic breast condition is a common benign (non-cancerous) breast condition related to the menstrual cycle. Some women with fibrocystic breasts experience cysts (accumulated packets of fluid), lumpiness, areas of thickening, tenderness, or breast pain. Symptoms of fibrocystic change will usually subside after menopause but may be prolonged if a woman uses hormone replacement therapy.
Women should continue monthly breast self-exams during pregnancy. It is especially important that a clinical breast exam be performed by the physician or nurse during the first doctor’s appointment of the pregnancy, before the breasts go through significant physiologic changes. Clinical breast exams should then continue on a monthly basis during pregnancy. Screening mammograms in asymptomatic women (women who have no symptoms of breast cancer) are not performed during pregnancy or lactation and may be performed at a later time.
During pregnancy, a variety of breast changes occur. Typically, breasts become tender and the nipples become sore a few weeks after conception. The breasts also increase in size very quickly. It is not uncommon for a woman’s breasts to increase by one or two cup sizes during and after pregnancy. The most rapid period of breast growth is during the first eight weeks of pregnancy. The Montgomery’s gland surrounding the areola (pigmented region surrounding the nipple) becomes darker and more prominent, and the areola itself darkens. The nipples also become larger and more erect as they prepare for milk production. The blood vessels within the breast enlarge as surges of estrogen stimulate the growth of the ducts and surges of progesterone cause the glandular tissue to expand.
Two hormones are responsible for milk production: prolactin and oxytocin. Prolactin is sometimes referred to as the "mothering hormone" because some people believe it also causes a tranquilizing effect that makes women feel more maternal. The body begins producing prolactin approximately eight weeks after conception. As the pregnancy progresses, the levels of prolactin steadily increase, peaking when the woman gives birth. As the body produces more and more prolactin, high levels of estrogen and progesterone block some of the prolactin receptors and inhibit milk production until after the baby is born.
After birth, estrogen and progesterone levels decrease and the production of prolactin declines. The breasts will usually begin to produce milk three to five days after a woman has given birth. During these few days before milk is produced, the body produces colostrum, a liquid substance that contains antibodies to help protect the infant against infections. Some physicians believe that colostrum also decreases an infant's chances of developing asthma and other allergies. Within a few days, the infant's own immune system will develop and he or she will not need colostrum.
The other hormone responsible for milk production, oxytocin, delivers the milk that prolactin has produced. When an infant suckles at the mother’s breast, it brings milk out of the nipples. This suction signals the body to make more milk (using prolactin) and deliver more milk (using oxytocin). The body also produces a variety of other hormones (insulin, thyroid, cortisol) that provide the infant with nutrition when he or she takes the mother’s milk. A woman’s body will continue to produce milk until she stops breast-feeding, and even then, it may take several months for milk production to completely stop. The breasts will usually return to their previous size (or slightly smaller) after breast-feeding is completed.
When a woman reaches menopause (typically in her late 40s or early 50s), her body stops producing estrogen and progesterone. The loss of these hormones causes a variety of symptoms in many women including hot flashes, night sweats, mood changes, vaginal dryness and difficulty sleeping. During this time, the breasts also undergo change. For some women, the breasts become more tender and lumpy, sometimes forming cysts (accumulated packets of fluid).
The breasts’ glandular tissue, which has been kept firm so that the glands could produce milk, shrinks after menopause and is replaced with fatty tissue. The breasts also tend to increase in size and sag because the fibrous (connective) tissue loses its strength. Because the breasts become less dense after menopause, it is often easier for radiologists to detect breast cancer on an older woman’s mammogram films, since abnormalities are not hidden by breast density. Since a woman’s risk of breast cancer increases with age, all women should begin receiving annual screening mammograms at age 40, and continue monthly breast self-exams and physician-performed clinical breast exams every year. Click here to learn more about breast cancer.
- For books on breast anatomy and physiology, please visit the Breast Health section of the Imaginis.com bookstore at http://www.imaginis.com/bookstore/
Updated: July 17, 2009



